肿瘤免疫组合疗法Opdivo/NKTR-214开展5种肿瘤治疗研究
2016-09-29 佚名 生物谷
肿瘤免疫治疗领域的绝对领跑者百时美施贵宝(BMS)近日宣布与Nektar制药公司达成一项新的临床合作,评估百时美的PD-1免疫疗法Opdivo(nivolumab)与Nektar公司的免疫刺激疗法NKTR-214的组合方案,用于5种肿瘤类型及潜在7个适应症。 Opdivo是一种PD-1免疫检查点抑制剂,旨在克服免疫抑制;NKTR-214则是一种免疫刺激疗法,旨在直接扩张肿瘤微环境中的特异性抗

肿瘤免疫治疗领域的绝对领跑者百时美施贵宝(BMS)近日宣布与Nektar制药公司达成一项新的临床合作,评估百时美的PD-1免疫疗法Opdivo(nivolumab)与Nektar公司的免疫刺激疗法NKTR-214的组合方案,用于5种肿瘤类型及潜在7个适应症。
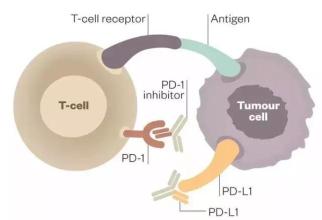
Opdivo是一种PD-1免疫检查点抑制剂,旨在克服免疫抑制;NKTR-214则是一种免疫刺激疗法,旨在直接扩张肿瘤微环境中的特异性抗癌T细胞和自然杀死细胞(NK),同时增加这些免疫细胞表面PD-1的表达水平。Opdivo与NKTR-214具有2种不同的、互补性的作用机制;将2者联合用药有望提高机体免疫系统对抗癌症的能力。
根据协议,双方将开展一项I/II期临床研究,评估Opdivo+NKTR-214组合疗法用于5种类型肿瘤(黑色素瘤、肾细胞癌、结直肠癌、膀胱癌、非小细胞肺癌),并与当前标准护理疗法进行对比。目前,一项初步的剂量递增试验正在进行中。百时美和Nektar将平摊临床开发成本,Nektar将保留NKTR-214的全球商业化权利。
NKTR-214能够增加体内肿瘤浸润性淋巴细胞(TILs)数量来补充免疫系统,这一点至关重要,因为许多患者因体内缺乏足够的TILs细胞群,导致难以从目前已获批的免疫检查点抑制剂中受益。将免疫检查点抑制剂联合T细胞增殖可能会产生协同作用,从而为患者提供一个新的治疗选择。
Opdivo是全球获批的首个PD-1免疫检查点抑制剂,于2014年7月获批上市,目前已在美国、日本、欧盟等54个国家获批上市。
NKTR-214是一种实验性药物,旨在靶向存在于CD8+效应T细胞和自然杀死细胞(NK cell)表面的CD122特异性受体,刺激体内的这些抗癌免疫细胞。在临床前研究中,NKTR-214治疗导致这些细胞快速扩张并动员到肿瘤微环境中去。NKTR-214具有抗体类药物的给药方式,与目前已获批的免疫检查点抑制剂药物给药方式相似。目前,Nektar公司正在开展一项I/II期研究,评估NKTR-214单药疗法治疗多种肿瘤的潜力。
原始出处:
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言












#组合疗法#
97
#NKTR-214#
74
#NKT#
82
文章很好,继续关注
116
#Opdivo#
71
#肿瘤治疗#
55